
Introduction
Millions of individuals throughout the world suffer with diabetes, a chronic illness. Many individuals are unaware of the potential problems that can result from untreated diabetes, despite the fact that it is well known for its effects on blood sugar levels and other organs. One such complication is gangrene, a potentially fatal condition brought on by diminished blood flow to tissues and capable of causing the death of bodily tissues. We will examine the causes, signs, and treatment options for gangrene as well as the connection between diabetes and gangrene in this blog post.
Having Diabetes Increases Your Risk of Gangrene
A condition called gangrene is characterized by the degeneration of bodily tissues as a result of inadequate blood flow.
This happens when blood arteries narrow or block, obstructing the flow of oxygen and nutrients to the affected tissues. Because it can result in a number of physiological changes that raise the possibility of decreased blood flow and nerve injury, diabetes is a significant risk factor for the development of gangrene. Following are some ways that diabetes feeds gangrene:
Poor Blood Sugar Control:
High blood sugar levels over time can damage blood vessels and impair
circulation, making it harder for blood to reach extremities like the feet and hands.

Peripheral Neuropathy:
Diabetes can damage nerves, a condition known as peripheral neuropathy.
When nerves in the extremities are affected, individuals may lose sensation, making it difficult
to detect injuries or infections.
Reduced Immune Function:
Diabetes can weaken the immune system, making it harder for the body to fight infections. Untreated infections can contribute to the development of gangrene.

Types of Gangrene in Diabetics
There are different types of gangrene, and diabetics are particularly prone to certain forms:
Dry Gangrene:
This type of gangrene typically occurs in extremities, such as the toes or fingers.
It progresses slowly and is characterized by dry, blackened tissue.
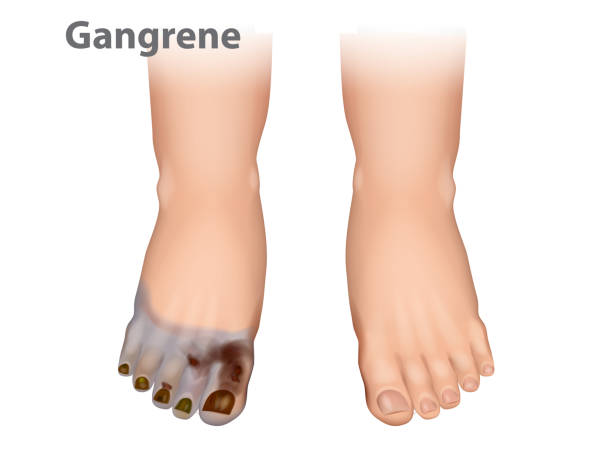
Wet Gangrene:
Wet gangrene is characterized by tissue that becomes moist and infected due to the
presence of bacteria. Diabetics are more susceptible to wet gangrene because of their compromised immune system.
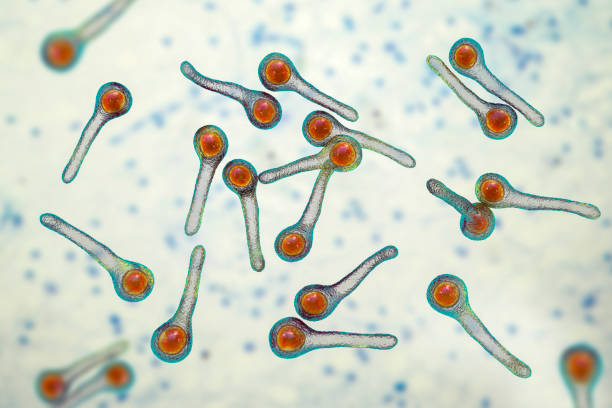
Gas Gangrene:
Gas gangrene is a rare but severe form of gangrene caused by bacterial infection.
It can spread rapidly and is a medical emergency.
Gangrene in Diabetics: Signs and Symptoms

Early intervention requires an understanding of the gangrene symptoms. The following signs of gangrene in diabetics could be present:
- Affected area discomfort, puffiness, or redness.
- Skin that darkens, going from light to blue to black.
- the affected area becoming numb or losing its sensitivity.
- the discharge from a wound that has an unpleasant smell or pus in it.
- In cases of wet or gas gangrene, fever and general malaise are present.
Management and Prevention
In order to avoid gangrene in diabetics, it’s important to control the underlying diabetes and practice proper foot hygiene:
Blood Sugar Control:
Use food, exercise, and, if required, medication to keep blood sugar levels within the goal range advised by your healthcare professional.
Foot care:
Look for cuts, sores, blisters, or redness on your feet every day. Wear cozy, well-fitting shoes and keep your feet dry and tidy.

Regular Check-ups:
Visit your healthcare provider regularly for diabetes management and foot exams.

Smoking Cessation:
If you smoke, quitting can improve circulation and reduce your risk of gangrene.
Wound Care:
Promptly treat any wounds or infections on your feet or extremities and seek medical attention if you notice any signs of gangrene.

Conclusion
Diabetes is a complicated disease that can affect many different parts of the body, increasing the risk of gangrene among them. Maintaining excellent overall health and preventing the development of this significant complication require understanding the connection between diabetes and gangrene, as well as taking preventive steps and treating diabetes efficiently. Develop a thorough plan for managing your diabetes and lowering your risk of gangrene by working together with your healthcare team.

